Personal Wealth Management / Economics
Pharma Vs. PBMs: Inside the US Government's Drug Price Reform Debate
While the debate is far from over, the early rumblings suggest to us potential drug price reform isn’t likely to materially affect Pharmaceuticals stocks.
Since 2016’s presidential campaign, political rhetoric fanning fears of major drug price regulation has weighed on sentiment toward Pharmaceuticals stocks. Those fears weren’t fulfilled during President Trump’s first two years, but many now argue the Democrats’ House victory in last year’s midterms changes the calculus, paving the way for Trump to push bipartisan prescription drug pricing reform. While small measures are possible, we think the big, sweeping drug price caps investors fear most are unlikely to pass. Limited reform tied to the Pharmacy Benefit Manager (PBM) rebate system seems more probably, and it likely lacks the scale to dent Pharmaceuticals’ earnings.
For those unfamiliar with the prescription drug supply chain, PBMs are essentially middlemen between drug companies and health plans. PBMs serve the health plans and, indirectly, patients the plans represent by negotiating drug prices on their behalf. The result is a list of covered drugs for the health plans they represent, known as the formulary list. In turn, drugmakers pay PBMs rebates in order to get included, which the PBM then returns to the health plan. This rebate system is key, as PBMs generate their revenue based partly on the volume of rebates and discounts they get for health plans, which they can retain, reinvest or use to lower patient costs. While terms vary among health plans, the standard industry presumption is that PBMs return approximately 90% of total rebate dollars to health plans and employers.[i] However, the system isn’t very transparent, and patients often don’t benefit directly from PBM rebates—surveys show health plans most often use the rebates to reduce their own costs rather than offset patient premiums or their out-of-pocket costs for prescriptions. (Exhibit 1)
Exhibit 1: How Health Plans Use PBM Rebates
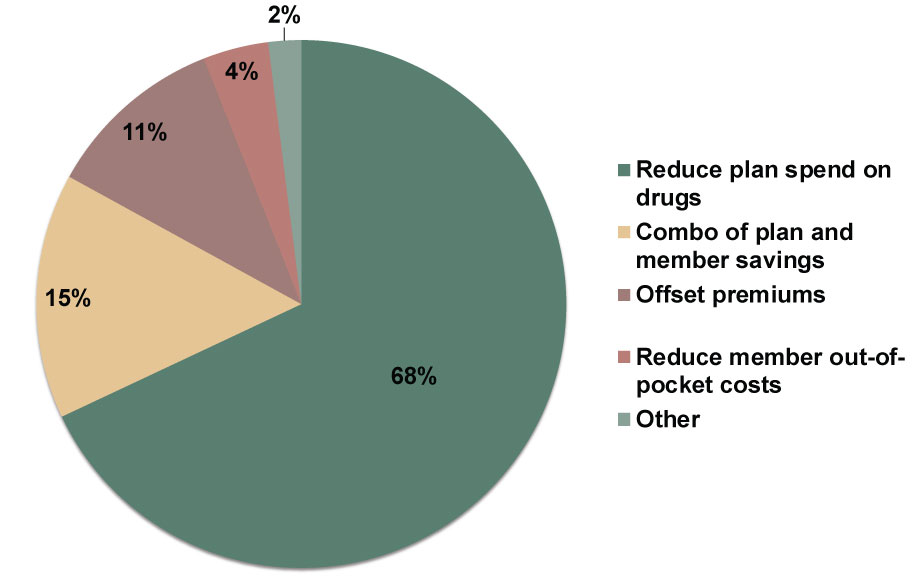
Source: Drug Channels Institute and Pharmacy Benefit Management Institute, as of 1/18/2018. Employers’ Use of Formulary Rebates, 2017.
Drug companies and PBMs often blame each other for high drug prices. Drug companies claim patients are stuck with high out-of-pocket costs when PBMs exclude drugs from their formulary lists. They go on to claim prices are so high because PBMs and health insurers want larger rebates—hence, drugmakers can’t just cut prices unilaterally. PBMs and health insurers claim rebates help patients, blaming drug companies for continuing to raise list prices. Recently, drug companies expanded their use of coupons and financial aid to try to lower patients’ cost, but PBMs and health plans pushed back, arguing these practices lead to higher use of more expensive, branded drugs. Both sides want Congress to focus on the other’s “abuses.”
This debate was in focus at the February 26 Senate Finance Committee hearing on drug pricing. Lawmakers questioned CEOs of seven major drug companies on why drug prices were so high. The CEOs pointed the finger at PBMs, arguing lowering list prices reduces rebates paid to PBMs, jeopardizing the drug’s position on formulary lists. The CEOs argued the drug rebate system creates conflicts of interest between health plans and patients, as insurers keep most of the rebate dollars rather than pass savings along to patients. AstraZeneca’s CEO went as far as to say said the company could dramatically reduce list prices if rebate reform passes. Of course, this is only one side of the story: PBMs will get their chance to point the finger at drug companies at a separate Senate hearing later this year.
So far, it looks like the Trump administration is taking drug companies’ side. President Trump’s drug pricing policy blueprint included a proposal to restrict and reduce PBM rebates in Medicare Part D. Further, the President has tweeted or commented on cutting out the “middlemen” in the prescription drug supply chain. Additionally, Trump’s Health and Human Services Secretary, Alex Azar, previously worked in the Pharmaceuticals industry. So did outgoing Food and Drug Administration Commissioner Scott Gottlieb. Their public comments have been critical of PBM rebates.
If the administration follows through with legislative or regulatory action targeting PBM rebates, PBMs’ and health insurers’ profits and revenues could suffer. However, Pharmaceuticals firms would likely see only a very limited impact. Perhaps lower overall drug prices result, but if potential legislation reduces or eliminates PBM rebates, that could mitigate the effect on Pharmaceuticals’ bottom lines, as they would keep a higher percentage of overall US drug spending. Rebates’ share of drug spending has been growing quickly the last few years, while net drug spending (i.e., what drug companies keep) has been relatively flat. (Exhibit 2)
Exhibit 2: PBMs and Health Plans Are Keeping a Larger Share of Drug Spending Through Rebates
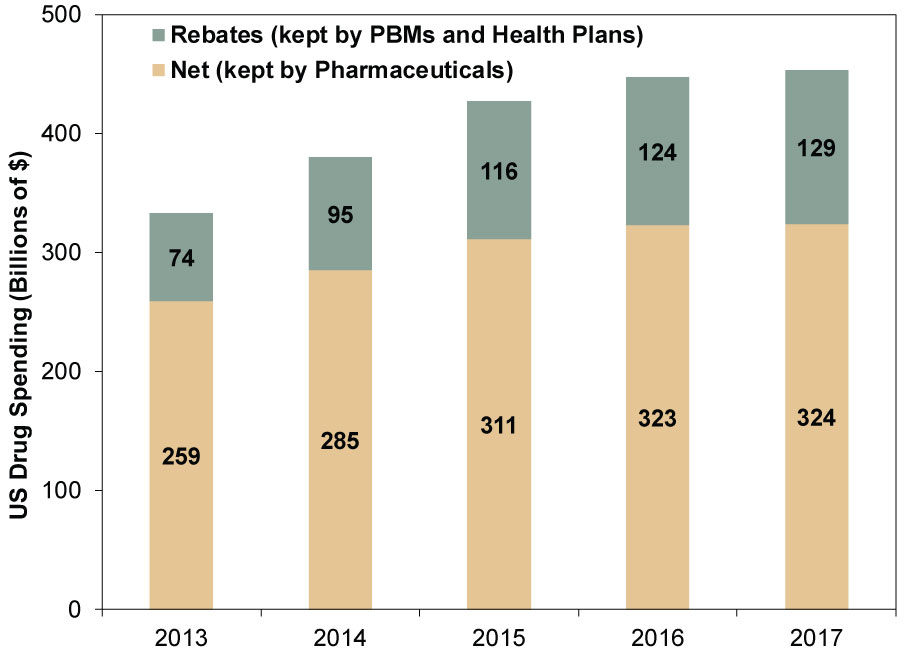
Source: “Medicine Use and Spending in the US,” IQVIA National Sales Perspectives, IQVIA Institute, April 19, 2018.
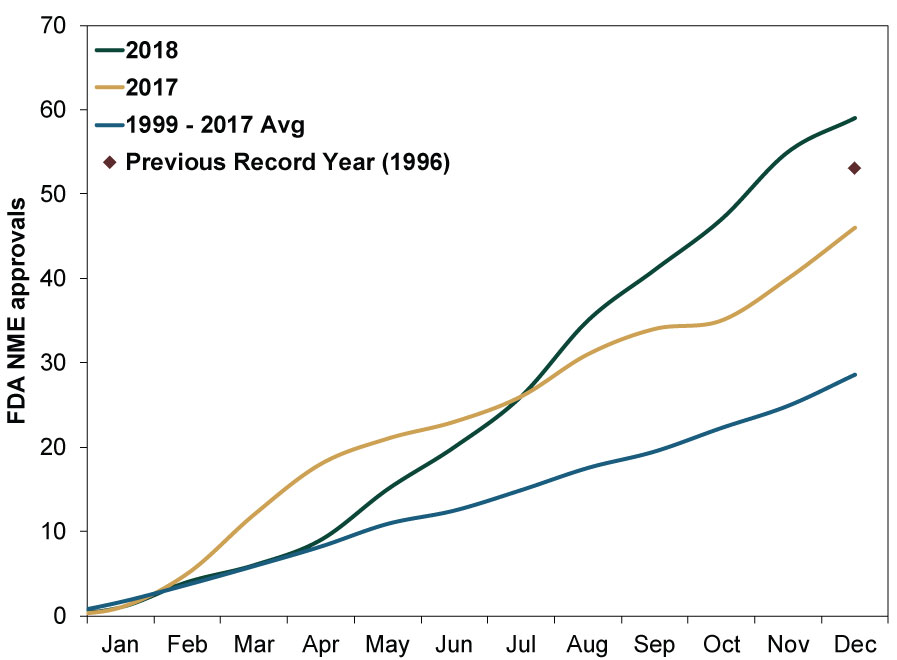
Meanwhile, the FDA has taken a different approach to reducing drug prices: increasing competition. December 2016’s passage of the 21st Century Cures Act led the agency to begin streamlining its approval process for new drugs and generics. Like any new law, this act creates winners and losers within the industry. Generic producers likely face headwinds from increased competition. However, brand-name Pharmaceuticals firms benefit from increased new drug approvals. This looser regulatory environment, coupled with strong drug innovation, led to the FDA’s approving a record 59 new drugs in 2018. (Exhibit 3) Protected for years by patents, these new drugs are key to future revenue and profit growth for innovative firms.
Exhibit 3: 2018 Set a Record for FDA Drug Approvals
Source: FDA, as of 12/31/2018.
While drug pricing likely stays in the headlines in the near term, a split Congress should water down any potential bill. If the current rumblings hold and PBM reform emerges, I would expect Pharmaceuticals stocks to respond favorably. While Pharmaceuticals may see price increases limited either by political pressure or actual pricing reform, this should be more than offest by increasing volume and new opportunities via drug approvals. These strong fundamentals could prove to be a potential positive surprise for investors just looking at fearful headlines claiming price controls lurk.
If you would like to contact the editors responsible for this article, please message MarketMinder directly.
*The content contained in this article represents only the opinions and viewpoints of the Fisher Investments editorial staff.
Get a weekly roundup of our market insights
Sign up for our weekly e-mail newsletter.

You Imagine Your Future. We Help You Get There.
Are you ready to start your journey to a better financial future?

Where Might the Market Go Next?
Confidently tackle the market’s ups and downs with independent research and analysis that tells you where we think stocks are headed—and why.